Politics Masquerading as Science 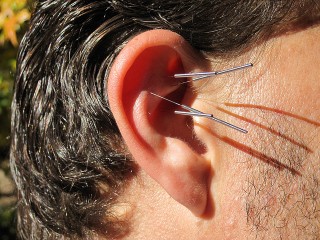
By Dr Stuart Jeanne Bramhall
I find it ironic how eager mainstream doctors are to condemn natural health treatments for not being “evidence-based.” Especially when Western medicine can produce little or no scientific evidence regarding the long term effectiveness and safety of many of their treatments. This is particularly true of heart surgery and immunization protocols. We operate on hearts and vaccinate kids for reasons that have nothing to do with scientific evidence. At the same time, we hold “natural” or “alternative” health providers to a much higher standard of proof. This is for complex political reasons that have given organized medicine and Big Pharma a virtual monopoly over health and healing. It has nothing to do with science.
The Myth of Evidence-Based Medicine
Doctors seem to forget that most common Western remedies were incorporated into the medical armamentarium centuries ago without any “proof” whatsoever of their effectiveness or safety. There were no randomized controlled trials when doctors began using digitalis for heart failure, morphine for pain, or sudafed for nasal congestion. All, like many other drugs, are plant-based treatments* originally used by midwives and herbalists (women the Catholic Church condemned as “witches”).
It was only when pharmaceutical companies began to develop synthetics substitutes that drugs were subjected to randomized control trials. Likewise, the long term outcome of many surgical interventions is never studied before they are rushed into the marketplace. A recent Wall Street Journal article examines the cost effectiveness of two common cardiac procedures – coronary angioplasty and coronary bypass surgery.
According to the article, in 2006 American surgeons performed 1.3 million coronary angioplasties at an average cost of $48,399 each – at a total cost of more than $60 billion. The same year they performed 448,000 coronary bypass operations at a cost of $99,743 each – at a total of more than $44 billion.
Despite these costs, a randomized controlled trial published in the New England Journal of Medicine found that angioplasties and stents don’t prolong life or even prevent heart attacks in stable patients (i.e. 95% of patients who receive them). Likewise coronary bypass surgery prolongs life in less than 3% of cases.
The Bias Against Natural Health Care
The authors ask: Why do Medicare and health insurance companies pay billions of dollars for dangerous, expensive, and largely ineffective heart surgeries – yet balk at paying for “natural” approaches that have proven to reverse and prevent the chronic diseases that account for at least 75% of health care costs (INTERHEART study, The Lancet, Sept 2004)?
Good question.
How “Natural” Treatments Affect Genes
The Wall Street Journal article mentions other research into the mechanism by which plant-based diets, yoga, and meditation halt or even reverse the progression of prostate cancer, heart disease, diabetes, hypertension, and other chronic conditions.
One study, published in the Proceedings of the National Academy of Science, provides evidence that only a few months of these “natural” treatments permanently alters gene expression. It describes how genes associated with cancer, heart disease, and inflammation were downregulated or “turned off,” while protective genes were upregulated or turned on.” Another study published in The Lancet Oncology reported that these changes also increased telomerase, the enzyme that lengthens the telomeres at the ends of our chromosomes. Telomeres control how long we live. No prescription medication has ever been shown to do this.
Popularity of Natural Health Care
A recent Discovery Channel special revealed that 40% of Americans employ use some form of “natural” medicine. At their website, they list the ten most common, in order of popularity, along with general comments about documented benefits and potential risks:
1. Natural supplements and herbal medicines – benefits best supported by research evidence include omega 3 for heart disease, arthritis, and depression; garlic for cholesterol reduction; and ginseng for heart disease. In the US, quality control can be a major issue with natural and herbal supplements, as they aren’t regulated and may contain heavy metals and other toxins. In New Zealand, the Natural Health and Supplementary Products Bill (awaiting its third reading) would establish standards for quality, strength, and purity.
2. Acupuncture – has the strongest evidence base, not only for pain relief, but to improve immunity and alleviate a range of chronic conditions. These are summarised in a recent World Health Organisation report. Some of the most common conditions that respond to acupuncture include rhinitis (runny nose – works better than antihistamines), sinusitis, asthma, irritable syndrome, hypertension, obesity, high cholesterol, menstrual cramps, migraine, menopausal symptoms, and stroke recovery (restores limb function).
3. Spinal manipulation (chiropractic) – also has a growing evidence base of effectiveness in chronic pain and other chronic illnesses.
4. Meditation – research supports effectiveness in treatment of anxiety, depression, and chronic pain.
5. Therapeutic massage – strong evidence base for therapeutic benefit in cancer, HIV, fibromyalgia, and other chronic pain conditions.
6. Ayurveda – an ancient Indian method of healing which shows promise as a way to boost memory and focus, though research into this approach is extremely limited. Some supplements used in this approach can contain heavy metals or cause dangerous interactions with prescription medication.
7. Guided imagery – demonstrated effectiveness in depression, anxiety, and pain.
8. Yoga – studies show that regular yoga practice reduces stress, eases depression, helps control high blood pressure and diabetes symptoms, helps reduce inflammation and asthma symptoms, reduce back pain, and improve heart function.
9. Hypnosis – shows promise for stress relief, pain management, headaches, dental pain and childbirth.
10. Homeopathy – very limited research base because the individualised treatments used make it hard to generate meaningful statistics.
The Role of Private Health Insurance
In the US, an increasing number of insurance companies provider coverage for “natural” or “alternative” health care – especially if it’s offered in conjunction with mainstream medical care. The jargon used for these mixed mainstream-alternative health models is “complementary” or “integrative” health care. Most insurance companies require that complementary and alternative medicine (CAM) providers seeking insurance reimbursement be represented by a professional body with a formal accreditation process. There is also an expectation 1) that the accreditation body will establish clear treatment standards and 2) that all funding will be evidence and outcome-based. In other words, CAM providers must demonstrate a treatment actually works to be eligible for funding.
Some analysts project that insurance coverage for natural health care will be even easier to access under Obamacare – at least for patients who can afford the higher premiums of silver, gold, and platinum plans. The uninsured and patients locked into Medicaid or bare bones bronze plans will be out of luck.
The requirement for natural health services to be “evidence based” has led to the creation of a number of natural health research databases. Three of the most popular are the Mayo Clinic Alternative Medicine database, the NIH Complementary and Alternative Medicine database, and the Cochrane Complementary Medicine.
The Mayo Clinic is a world famous “mainstream” medical center in Minnesota. In my opinion, their database is by far the most comprehensive and user-friendly. I find the NIH and Cochrane databases less helpful. Both seem quite biased towards mainstream medicine and randomized controlled trials (RCTs). Many alternative treatment methods don’t lend themselves to RCTs because it’s virtually impossible to provide “sham” treatment (e.g. sham acupuncture, cupping, or aromotherapy) for the placebo group. Both NIH and Cochrane ignore the abundance of crossover design CAM studies in which the patient serves as their own control. In these studies, treatment is withdrawn once a clear response is established. When symptoms recur, it’s reintroduced. If patients respond a second time – and the sample is large enough to be statistically significant – this is taken as “proof” of effectiveness
*Below are just a few common medicines based on ancient plant-based treatments:
- Aspirin
- Atropine
- Curare
- Theobromine
- Taxol
- Scopolamine
- Reserpine
- Quinidine
- Quinine
- Papavarine
- Physostigmine
- Papain
- L-dopa
- Hyoscyamine
photo credit: SuperFantastic via photopin cc
Dr. Bramhall is a retired American child and adolescent psychiatrist, activist and political refugee in New Zealand.
Her first book The Most Revolutionary Act: Memoir of an American Refugee describes the circumstances that led her to leave the US in 2002. She has also published two young adult novels about political activism: The Battle for Tomorrow: A Fable
View All Books by Dr. Bramhall >>>
She is involved in the national leadership of the New Zealand Green Party and has a political blog at StuartJeanneBramhall.com
ATTENTION READERS
We See The World From All Sides and Want YOU To Be Fully InformedIn fact, intentional disinformation is a disgraceful scourge in media today. So to assuage any possible errant incorrect information posted herein, we strongly encourage you to seek corroboration from other non-VT sources before forming an educated opinion.
About VT - Policies & Disclosures - Comment Policy



