 GOUT: WHAT YOU NEED TO KNOW
GOUT: WHAT YOU NEED TO KNOW
BY CAROL DUFF RN
Gout is a painful and common type of arthritis. One out of 100 will develop gout at some point. Gout is the most common cause of inflammatory arthritis in men over 40.This malady has been around for centuries and is one of the earliest described conditions which still plague humanity.
There is an increasing prevalence of gout in the past decades which reflects an increasing health burden. The more developed countries have more incidences of gout due to a richer diet. As an area improves in ability to attain foods that would contain purines there will be more gout diagnoses.
Typically gout is associated with abnormally high amount of uric acid in the blood (hyperuricemia). With early intervention, careful monitoring, and patient education gout can be managed effectively…
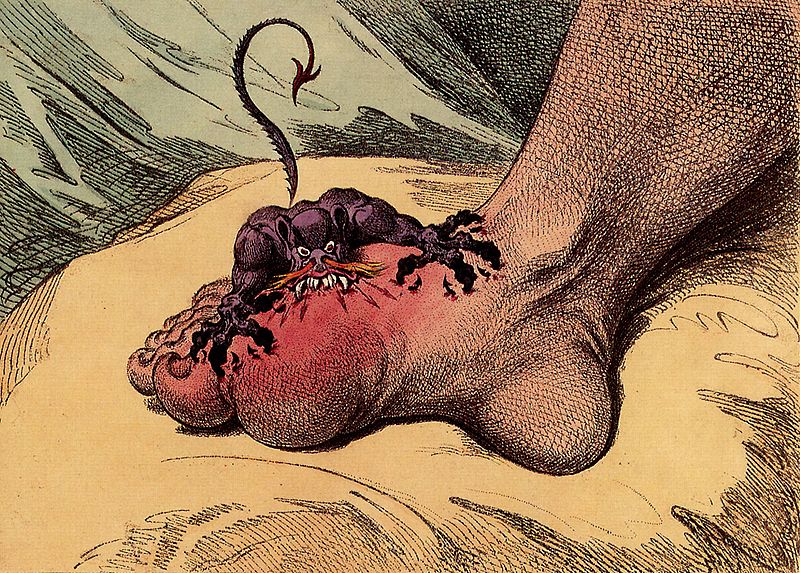
What Does Gout Look and Feel Like?
About two thirds of those who have gout state that it is the worst pain they have experienced. A flair up of gout can make walking difficult and putting on shoes nearly impossible.
Symptoms of a gout attack include:
-
Severe pain at and around a joint, usually on one side of the body. Sixty percent of middle aged people experience the first attack in the large toe. In the eldelry joints will be involved in the arms, hands, and especially the fingers.
-
The affected part may feel as though a bone is dislocated or crushed. Walking and even the weight of bed sheets may be unbearable· Gout usually takes between 8 and 12 hours to develop and may awaken you in the night or in the early morning.
-
There may be swelling of the area affected that extends beyond the joint. The skin area over the affected area may be red, shiny, and tight and may peel within a few days.
-
Loss of appetite, chills, mild fever, and just plain feeling lousy may accompany the gout attack.
There are two types of types of gout; primary and secondary. Primary gout has an unknown cause but in all likely hood is the result of a combination of genetic (others in the family have gout), hormonal, and dietary factors. Secondary gout is caused by medications or medical conditions which increase the blood levels of uric acid.
Cause
The cause of gout and hyperurecemia is the metabolism of purines which are nitrogen-containing compounds important for energy. Purines come from two sources:
-
Made in human cells (endogenous)
-
From foods (exogenous)
When the body breaks down purines uric acid forms, but in humans uric acid is not easily removed from the body. Other mammals have an enzyme (uricase) which breaks down uric acid so it can be removed and not build up in the body tissues.
Purines in the liver produce uric acid which then enters the bloodstream and eventually should go through the kidneys and be excreted in urine. The remainder of the uric acid moves through the intestines where bacteria break it down.
Usually the level of uric acid in the blood will be below the level of 6.8 mg/dL, but under certain circumstances the body either produces too much uric acid or removes too little. The level of uric acid rises in the blood and the diagnosis of hyperurecemia is made.
When uric acid reaches the level of 7mg/dL, crystals form which resemble needles and create a salt (monosodium urate [MSU]). These crystals build up in joints and cause the typical symptoms of pain and inflammation.
Sources of Purines
Activities that increase energy demands will also increase metabolism and the production of purines which produce uric acid. Staying healthy and avoiding stress are important preventative measures.
Uric acid levels are mildly affected by diet, so dietary therapy does not have a key role in preventing gout. With that said, it is still in your best interest to avoid foods high in purine if you have had a gout attack.
Foods high in purines are certain types of meats, seafood, and shellfish. Purine rich vegetables such as spinach, mushrooms, legumes, and cauliflower do not cause gout when consumed in moderate amounts do not increase the risk of gout.
Low fat dairy products such as low-fat yogurt and skim milk may actually protect against gout.
Foods to be avoided:
-
Organ meats (liver, kidneys, sweetbreads
-
Red meat (beef, pork, lamb)
-
Meat extracts (soup, broth, gravies)
-
Seafood (anchovies, sardines, herring, fish roe, canned tuna fish, shrimp, lobster, scallops, mussels
-
Yeast products (beer and baked goods)
Maintain a healthy weight with a supervised weight-loss program may be an effective way to reduce uric acid levels. Crash dieting is harmful because there can be an increase of uric acid levels and an acute attack may occur.
Fluids: Drink plenty of water and nonalcoholic beverages which will help to remove uric acid crystals from the body.
Alcohol promotes purine metabolism and uric acid production and may reduce the excretion of uric acid. Heavy drinking, especially binge drinking of beer and spirits, should be avoided
How Does Alcohol Increase Uric Acid Levels?
Alcohol provides purines from which uric acid is formed.·
Alcohol increases the body’s production of uric acid.·
Alcohol interferes with the kidney’s ability to excrete uric acid.
Risk Factors:
-
Increasing age, usually after 40·
-
Male
-
A family member has or has had gout·
-
Obesity (not always the case).
-
Use of certain drugs:
Diuretics (help to loose excess water in body)
Aspirin
Cyclosporine (an immunosuppressant drug used after transplant surgery to decrease chance of organ rejection)
Levodopa (used to increase missing dopamine in those with Parkinson’s disease and has also been used for many years as an effective treatment for restless leg syndrome (RLS).
-
Drinking a large amount of alcohol, particularly beer.
-
Exposure to lead.
-
Thyroid problems
-
Organ transplants
Triggers of Gout
Triggers are events or conditions that can set off a gout attack. Certain risk factors, including a purine-rich diet, are also considered a trigger. Triggers include:
-
Joint injury
-
Overindulging in alcohol or purine-rich foods
-
Over strenuous exercise
-
Severe illness or infection
-
Stress
-
Sudden weight loss
-
Surgery
-
Using certain drugs
Hot and humid weather is associated with attacks of gout. Excessive sweating leads to dehydration which is a trigger for a gout attack. The August 2006 journal, Arthritis and Rheumatism, states that gout is linked to an increase risk of heart attacks in men who have previously had no heart problems.
Many who experience gout do not require medications but that decision if up to your healthcare provider. Between gout attacks avoid food that are high in purines, reach a healthy weight, avoid alcohol use and reduce stress.
Make Yourself More Comfortable
-
Use pillows to build a “frame” to keep bed linens and
blankets off the painful joints when lying in bed.
-
Allow the joints to rest.
-
Drink 10 to 12 glasses of water each day to try to
prevent kidney stones.
Avoid Joint Injury: Avoid activities which causes repetitive joint trauma, even wearing tight shoes is trauma.
Untreated gout can develop into a disabling chronic disorder and can in time destroy cartilage and bone and cause loss of motion and joint deformities that cannot be fixed.
When your healthcare provider treats your gout he or she will either try to reduce inflammation in acute gout, or try to prevent gout with measures that manage hyperuricemia. There are non-pharmaceutical interventions such as lifestyle modifications to diet with a minimum intake of foods that produce purines, weight control, and decreased alcohol consumption.
You must immediately see your healthcare provider if you suspect you are experiencing the symptoms of gout. Acute attacks will be treated with anti-inflammatory drugs, but it must be recognized that underlying hyperuricemia exists. Urate-lowering drugs should be monitored to achieve a serum level of less than 6.0 mg;dL (360 mmol/L)
Your health care provider will prescribe the drug to lower the uric acid level in the blood. Anti-inflammatory drugs may shorten acute attacks and relieve pain but that is determined from patient to patient.
Possible urate lowering therapy.
Life style, diet, and other diseases such as arthritis, diabetes, and heart disease should be evaluated.
People with chronic gout may benefit from medications that lower uric acid levels.
New therapies are under development for those cases that are difficult to manage.
Your healthcare provider will determine which medications you should take.
Remember, there is evidence of under treatment, over treatment, and inappropriate medication use in patients with gout.
Be involved in your healthcare and ask questions. A helpful hint is to write your questions down before you go to your appointment so you will remember everything you wish to discuss with the healthcare provider.
Getting health care as soon as you suspect you may have gout will improve your chances of getting a grasp on gout. The sooner the treatment, the sooner you will feel better.
References
Chen, L.X., and Schumacher, H.R. (2006). Gout: Can we create an evidence-based systematic approach to diagnosis and management? Best Practices and Research Clinical Rheumatology 20 (4), p. 673-684.
Health Library, in Depth reports-gout Walgreens.mht
Krishnan E, Baker JF, Furst DE, Schumacher HR. Gout and the risk of acute myocardial infarction. Arthritis Rheum. 2006 Aug;54(8):2688-96.
Jelley, M.J. and Wortmann, R. (2000). Practical steps in the diagnosis and management of gout. Biodrugs August 14 (2), p. 99-107.
Nuki, G. (2006). Gout: Metabolic and genetic anomalies. Medicine 34 (10), p. 417-422.
Sing, J.A., Hodges, J.S., Toscano, J.P., and Asch, S.M. (2007) Quality of care for gout in the US needs improvement. Arthritis & Rheumatism (Arthritis Care & Research) 57 (5), p. 822-829.
YQ Zhang, Chaisson CE, Chen CA, McAlindon TE, Hunter DJ. High Humidity and High Temperature Increase the Risk of Recurrent Gout Attacks: The Online Case-crossover Gout Study. Presentation Number 707. American College of Rheumatology Annual Scientific Meeting, Washington, DC, November 2006.
Teng, G.G., Nair, Raj, Saag, K.G. (2006). Pathophysiology, clinical presentation and treatment of gout. Drugs 2006, 68 (12), p. 1847-1963.

Carol graduated from Riverside White Cross School of Nursing in Columbus, Ohio and received her diploma as a registered nurse. She attended Bowling Green State University where she received a Bachelor of Arts Degree in History and Literature. She attended the University of Toledo, College of Nursing, and received a Master’s of Nursing Science Degree as an Educator.
She has traveled extensively, is a photographer, and writes on medical issues. Carol has three children RJ, Katherine, and Stephen – one daughter-in-law; Katie – two granddaughters; Isabella Marianna and Zoe Olivia – and one grandson, Alexander Paul. She also shares her life with her husband Gordon Duff, many cats, and two rescues.
ATTENTION READERS
We See The World From All Sides and Want YOU To Be Fully InformedIn fact, intentional disinformation is a disgraceful scourge in media today. So to assuage any possible errant incorrect information posted herein, we strongly encourage you to seek corroboration from other non-VT sources before forming an educated opinion.
About VT - Policies & Disclosures - Comment Policy